Patient Safety in Dentistry: Managing Adverse Events in the Practice Setting
This article, the final installment of a three-part series on patient safety in dentistry, will address the management of adverse events in a dental practice.
The Agency for Healthcare Research and Quality (AHRQ) defines an adverse event as “harm from medical care rather than an underlying disease.”1 Adverse events are typically divided into three categories: preventable, ameliorable, and negligent. Preventable adverse events are those in which the harm may have been lessened or prevented had patient safety risk mitigation strategies been applied. An example of a mitigation strategy is checking for allergies before administering medication. When a clinician administers or prescribes medication despite a known allergy, the patient’s allergic response is considered a preventable adverse event. An ameliorable adverse event is one that, while not entirely preventable, may have resulted in less harm if the care had been provided differently, such as observing and monitoring a patient after administering anesthesia or sedation to ensure a rapid response to any complication. A negligent event involves a breach in the standard of care resulting in harm, when the breach is the direct cause of the harm. Determination of negligence often involves a judicial or regulatory process or both.
Florida dental regulations use two different terms, defined almost identically, for an adverse event. They use adverse incident and adverse occurrence:
Section 466.017(14) of the Florida Statutes includes the term adverse incident and defines it as “any mortality that occurs during or as the result of a dental procedure, or an incident that results in a temporary or permanent physical or mental injury that requires hospitalization or emergency room treatment of a dental patient which occurs during or as a direct result of the use of general anesthesia, deep sedation, moderate sedation, pediatric moderate sedation, oral sedation, minimal sedation (anxiolysis), nitrous oxide, or local anesthesia.”2
The Florida Board of Dentistry uses the term adverse occurrence, which it defines as “any mortality that occurs during or as the result of a dental procedure, or an incident that results in the temporary or permanent physical or mental injury that requires hospitalization or emergency room treatment of a dental patient that occurred during or as a direct result of the use of general anesthesia, deep sedation, moderate sedation, pediatric moderate sedation, minimal sedation, nitrous oxide, or local anesthesia.”3
These definitions focus on events in which a patient dies during or as a result of a dental procedure and any condition that requires patient hospitalization or emergency room treatment as the result of the use of any anesthesia, including local anesthetics. The opportunity for patient harm in dentistry is not limited to patients who have received anesthesia and sedation. This article will examine dental patient safety from the broader perspective of adverse event.
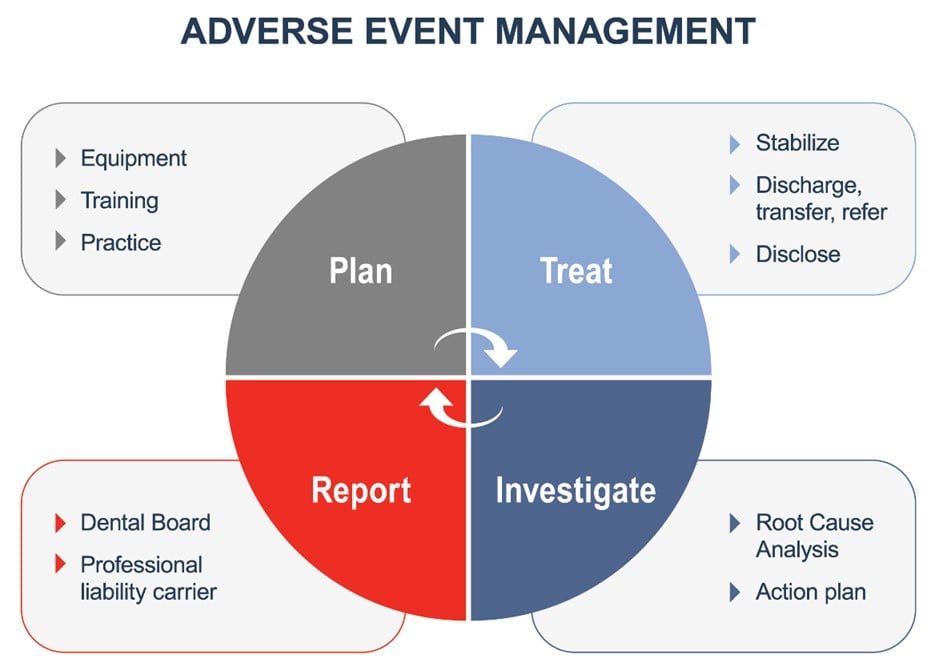
When an adverse event occurs in a dental practice, providers and staff must be prepared to respond appropriately. Preparations include developing response plans for the different types of emergencies that may occur, maintaining emergency equipment and supplies, role-specific training for staff members, and conducting periodic drills to identify process gaps. A well-managed adverse event response includes caring for the patient, investigating what happened, taking corrective action where needed, and reporting the event appropriately as required.
Take Care of the Patient
If an adverse event occurs, patient care takes precedence. Dentists and clinical staff must be prepared to manage the clinical situation. Involve emergency services as necessary. Consider conducting a brief huddle once the patient is stable for discharge or transfer. Assign someone to take notes and ask each participant to describe the event from their perspective. When time permits, consolidate the notes and initiate the investigation step. Keep the notes in an incident file that is separate from the patient’s record.
Sometimes an adverse event is discovered after treatment has occurred and the patient has left the office. Consider the following example:
Dr. Jones’ office received a request for records from a patient scheduled to see an oral and maxillofacial surgeon (OMS). As was customary in the office, Dr. Jones was made aware of the request and looked over the records to ensure that the office staff had pulled everything the OMS would need. Dr. Jones had seen the patient for an infected tooth and performed a root canal and crown placement. The patient healed well and had not called the office or returned for additional care. When Dr. Jones re-reviewed the initial radiography image files taken before the root canal, she noted a finding not previously appreciated. She saw a hairline fracture of the mandible from the area below the treated tooth into the mandibular angle.
Dr. Jones contacted the OMS immediately to discuss the findings. She and the OMS suspected infection and nonunion of the mandibular fracture. The patient had been scheduled for a nonurgent examination to assess pain and reduced jaw movement. The OMS office contacted the patient and rescheduled an earlier appointment.
In this case, both the delayed diagnosis of the fractured jaw and the infection were adverse events. The pain and decreased jaw mobility from the infection may have been preventable. If Dr. Jones had noted the fracture, she would likely have delayed surgical management of the infected tooth to treat the mandibular fracture.
Dr. Jones recognized the necessity of communicating the missed finding to the OMS. Admitting professional errors to a colleague, though challenging, demonstrates integrity. Notifying the downstream provider also reduces the risk of nonprofessional communication (refer to Part 1 of this series).
Dr. Jones must also advise the patient of the missed fracture. Communicating adverse events to patients and families, or disclosure, is an ethical obligation. Disclosing represents the principle of respect for autonomy. In the case above, disclosure to the OMS represents nonmaleficence. Although the OMS would likely have noted the fracture, contacting the OMS and discussing the context are essential to ensure patient safety.
Trust is a vital component of the provider-patient relationship. Anything that erodes this trust puts both parties at risk. While it may seem counterintuitive at first, notifying patients and families when an adverse event occurs may improve the provider-patient relationship if it is done well.4 From a professional liability perspective, it is unclear whether disclosure prevents claims, primarily because it is difficult to measure something that does not happen. Subjective evidence suggests that patients may be more forgiving when providers offer an honest and sincere disclosure and apology. Literature supports the notion that providers with poor communication skills who appear insensitive or untruthful are more likely to be sued by patients and families.5
In Florida, as in many states, disclosure is a legal obligation:
Every licensed health care practitioner shall inform each patient, or an individual identified pursuant to s.765.401(1), in person about adverse incidents that result in serious harm to the patient. Notification of outcomes of care that result in harm to the patient under this section does not constitute an acknowledgment of admission of liability, nor can such notifications be introduced as evidence.6
Also known as the “Duty to Notify,” this statute applies to all licensed healthcare practitioners, including dentists. Providers who fail to disclose are at risk for professional board disciplinary action.
At some point, every dentist will face the difficult decision about disclosure. When making treatment decisions, use an objective, rational, and patient-centered decision-making process, much like every provider’s risk-benefit analysis. The following simple guidelines may also be helpful: Disclose an adverse event if it (1) causes or has the potential to cause harm, (2) requires additional treatment or monitoring, or (3) would affect your desire to know if it happened to you or a relative. Disclosure is usually best managed face to face. Ideally, the patient would come to the practice; however, it is possible to have an effective disclosure discussion virtually using telehealth. Plan ahead for questions that the patient might ask and for possible emotional behaviors. Avoid becoming defensive. Explain objectively what happened, avoid blaming others, and do not speculate. Be honest and sincere.
An empathetic apology may be very helpful to both parties. Because disclosure is required and so many healthcare professionals are concerned about liability, most states—including Florida—protect disclosure discussions from discovery and use in a malpractice claim:
The portion of statements, writings, or benevolent gestures expressing sympathy or a general sense of benevolence relating to the pain, suffering, or death of a person involved in an accident and made to that person or to the family of that person shall be inadmissible as evidence in a civil action. A statement of fault, however, which is part of, or in addition to, any of the above shall be admissible pursuant to this section.7
At some point, admitting fault and offering compensation may be appropriate. To protect the practice, involve an attorney or your professional liability carrier before doing so. Document the discussion objectively in the dental record. Include date and time, location, a brief description of the discussion (including questions and answers), and patient and family responses.
Often, patients and families also want to know why the event happened to them and what will be done to prevent similar occurrences. Depending on the timing of the initial disclosure, these questions may not be answerable. After the event investigation, follow up with the patient and family to discuss actions taken. Keep the discussion at a high level and do not address confidential human resource actions.
Investigate the Event
Investigating an adverse event is very similar to making a diagnosis. Review the dental record information available at the time of the incident. Gather the staff members present during the incident (as appropriate) and walk through the process of care. Depending on the severity and complexity of the incident, it may be helpful to create a timeline. Look for factors and gaps that may have contributed to the adverse event and think about mitigation strategies that could have helped reduce the extent of or prevent the event. This process is called a root cause analysis (RCA). Use standardized tools (such as the Five Whys tool, a “fishbone” diagram, or a cause and effect tree) to ensure that you identify the root causes. Adverse events are rarely entirely attributable to a single individual. Do not use the RCA process to shame or blame an individual. Instead, look for system issues that may have led the individual to make a poor selection or forget a step. Typically, system factors contribute to an error-prone environment. Common contributing factors include distraction and interruption, overly complicated processes, lack of training, poor teamwork, and time pressure. Evidence-based tools and guidelines are available to assist in the process. See the resource list at the end of the article.
Use the investigation to identify the main contributing factors (root causes), prioritize them, and develop an action plan. Plans have better outcomes when specific team members take responsibility and have accountability for each corrective action. In the case example, Dr. Jones missed a mandibular fracture. Reduce the chances of missing a significant finding by ensuring that the most recent images are on a viewing screen in the treatment room. Add a second layer of patient safety by including a final image review on a preprocedure checklist. Assign responsibility for ensuring the images are up in the treatment room and review the checklist with the treatment team prior to proceeding with the treatment.
Once the plan is developed, circle back with the family. Thank them again for their patience and understanding and give a high-level overview of the plan. In the case example, Dr. Jones might state that, in the future, images will be placed in the treatment room for every procedure and the practice will use a checklist.
Report the Event If Required
Not all events that happen in a dental office require regulatory reporting. Patient deaths that occur during or as a direct result of a dental procedure must be reported to the Florida Board of Dentistry regardless of when the patient expires. It must also be reported to the board if a patient suffers a temporary or permanent physical or mental injury that requires hospitalization or treatment in an emergency department and the injury occurred during the use of anesthesia or as a direct result of the use of anesthesia.
Here is an example: A patient suffers a cardiac event in the office during a dental procedure and is transferred to a hospital. If the patient recovers and no form of anesthesia was used during the dental treatment, the transfer of the patient to the hospital does not meet the specific criteria for reporting. On the other hand, the event must be reported if the patient expires. If any form of anesthesia was used—including a local anesthetic—the event must be reported, regardless of whether the patient recovers.
The dental statute and rule concerning adverse events are very specific, and they apply to dentists (and any dental hygienist registered to administer local anesthesia) when administering local anesthesia. If an event is required to be reported, an initial report is due within 48 hours of the incident, with a follow-up report due within 30 days of the incident. A failure to timely report an adverse event can form a basis for discipline.
When a dentist is in doubt about whether to report an event to the Florida Board of Dentistry, the dentist should consult with legal counsel or a qualified risk manager.
Any event reported to the Florida Board of Dentistry should also be reported to the dentist’s professional liability carrier. It is essential to read insurance policy documents and be familiar with the requirements, including reporting. Although every insurance policy has nuances, patient harm that can result in a claim (sometimes known as a potentially compensable event, or PCE) is always reportable. PCEs in a dental office include but are not limited to death, diminished life expectancy, loss or impairment of an organ or sense, and disfigurement. Other actions by the patient or family or communications from an attorney or regulatory body are also reportable. These include written or verbal demands for money or threats of legal action by a patient or family, notices of legal action from a court or law firm, and requests to participate in a legal activity such as arbitration or a deposition. Failure to report an occurrence according to the policy terms may affect coverage if the event is litigated.
Most professional liability carriers have a patient safety or risk management department that can provide guidance on adverse events, reporting, and other patient safety topics.
Patient safety in dentistry is just as important as it is in any other field of medicine. Though dental patient safety science is still emerging, dental associations and regulatory boards have recognized and addressed the importance in the form of guiding principles and regulations. The rest is up to you.
As the authors of “Safety in Dentistry” note:
Ultimately, patient safety, like politics, is local. Leaders of individual practices must not only decide to allocate resources to patient safety activities within a dental practice, they must also cultivate an environment in which individuals feel that talking about patient safety concerns is valued.8
See the other articles in this series, “Patient Safety in Dentistry: Communication” and “Patient Safety in Dentistry: Documentation.”
Resources
National Patient Safety Foundation. RCA2: Improving Root Cause Analyses and Actions to Prevent Harm. Boston, MA: National Patient Safety Foundation; 2015. (Registration required.) http://www.ihi.org/resources/Pages/Tools/RCA2-Improving-Root-Cause-Analyses-and-Actions-to-Prevent-Harm.aspx
Minnesota Department of Health. Root Cause Analysis Toolkit. See Graphic Organizers/Diagrams. https://www.health.state.mn.us/facilities/patientsafety/adverseevents/toolkit/
References
- Agency for Healthcare Research and Quality. Patient safety 101. Adverse events, near misses, and errors. PSNet. September 7, 2019. Accessed March 30, 2022. https://psnet.ahrq.gov/primer/adverse-events-near-misses-and-errors
- Florida Statutes. 2021. §466.017(14). Accessed March 30, 2022.
- Florida Administrative Code. 2022. Chapter 64. Rule 64B5-14.006 Reporting Adverse Occurrences. Effective March 10, 2020. Accessed April 8, 2022.
- Chamberlain CJ, Koniaris LG, Wu AW, Pawlik TM. Disclosure of “nonharmful” medical errors and other events: duty to disclose. Arch Surg. 2012;147(3):282–286. Accessed March 30, 2022. doi:10.1001/archsurg.2011.1005
- Levinson W, Roter DL, Mullooly JP, Dull VT, Frankel RM. Physician-patient communication. The relationship with malpractice claims among primary care physicians and surgeons. JAMA. 1997;277(7):553–559. Accessed March 30, 2022. https://pubmed.ncbi.nlm.nih.gov/9032162/
- Florida Statutes. 2021. Title XXXII, §456.0575 (1) Duty to notify patients. Accessed March 30, 2022.
- Florida Statutes. 2021. Title VII, §90.4026 (2) Statements expressing sympathy; admissibility; definitions. Accessed March 30, 2022.
- Ramoni RB, Walji M, Kalenderian E. Agency for Healthcare Research and Quality. Safety in dentistry. PS Net. August 1, 2016. Accessed April 5, 2022. https://psnet.ahrq.gov/perspective/safety-dentistry
Reprinted with permission from Florida Focus. June 2022. Online ahead of publication. Will be available here: https://www.flagd.org/florida-focus/.
The guidelines suggested here are not rules, do not constitute legal advice, and do not ensure a successful outcome. The ultimate decision regarding the appropriateness of any treatment must be made by each healthcare provider considering the circumstances of the individual situation and in accordance with the laws of the jurisdiction in which the care is rendered.
J13454D 06/22
