What is the common factor in these cases?
- A 56-year-old female with a body mass index (BMI) of 54.1 experienced a fall that caused a complete transection of her popliteal artery and damage to the tibial nerve. A general surgeon failed to diagnose and treat the severed popliteal artery, which resulted in an above-knee amputation.
- A patient weighing more than 350 pounds suffered nerve damage due to positioning on a treatment table.
- A 46-year-old female with obstructive sleep apnea (OSA), morbid obesity (BMI 48.8), and hypertension was given Dilaudid to treat severe pain. She suffered respiratory arrest and died, allegedly due to inadequate monitoring by her nurses.
- A young male, 5 feet tall, weighing 290 pounds, elected to undergo gastric bypass surgery. Multiple post-op complications resulted in organ failure and led to his death two weeks later.
- A 35-year-old patient, 5 feet 4 inches tall, weighing 260 pounds, vomited and aspirated during a manipulation under IV sedation. No endotracheal tube was in place.
The common factor in these cases is evident: Each case had obesity-related complications in otherwise routine clinical settings.
Population Growth
Our population is continually growing—both in numbers and in size. The World Health Organization (WHO) defines overweight and obesity as “abnormal or excessive fat accumulation that may impair health.” BMI is a screening tool that is commonly used as a measure of overweight and obesity. It is a calculation of weight in kilograms divided by height in meters squared (kg/m2).
The WHO parameters for adults are:
- Overweight—a BMI equal to or greater than 25.
- Obesity—a BMI equal to or greater than 30.
Obesity is not restricted to adults; children are at risk as well. According to WHO statistics, in 2019, an estimated 38.2 million children under the age of five years fit the criteria for being overweight or obese.
The extent of obesity in the United States is indicated on the Centers for Disease Control and Prevention (CDC) Adult Obesity Prevalence Maps. In 2018, all states and territories had a prevalence of adults with obesity of 20 percent or greater.
Obesity-Related Claims Analysis
The Doctors Company continues to see an increase in lawsuits involving patients with obesity. Our analysis focused on obesity-related claims from 2011 through 2018. Of 17,910 closed claims coded during this time, patient obesity affected the outcome of care in 1,490 (8.3 percent) of the claims.
(Note: The incidence of obesity in the American population is much higher than the frequency in coded claims. Obesity and other comorbidities are coded only when they are viewed as having affected the outcome of care.)
The study compared claims in which obesity was a comorbidity that affected the outcome of care with claims in which obesity was not a comorbidity.
Paid Claims
The percentage of paid claims with no obesity comorbidity equaled 28.6 percent. The percentage of paid claims with an obesity comorbidity was slightly higher at 30.0 percent.
Patient Age and Gender
We evaluated all claims to determine the patient’s age when obesity affected the outcome of care. The chart below shows the number of claims with an obesity comorbidity by patient age and gender.
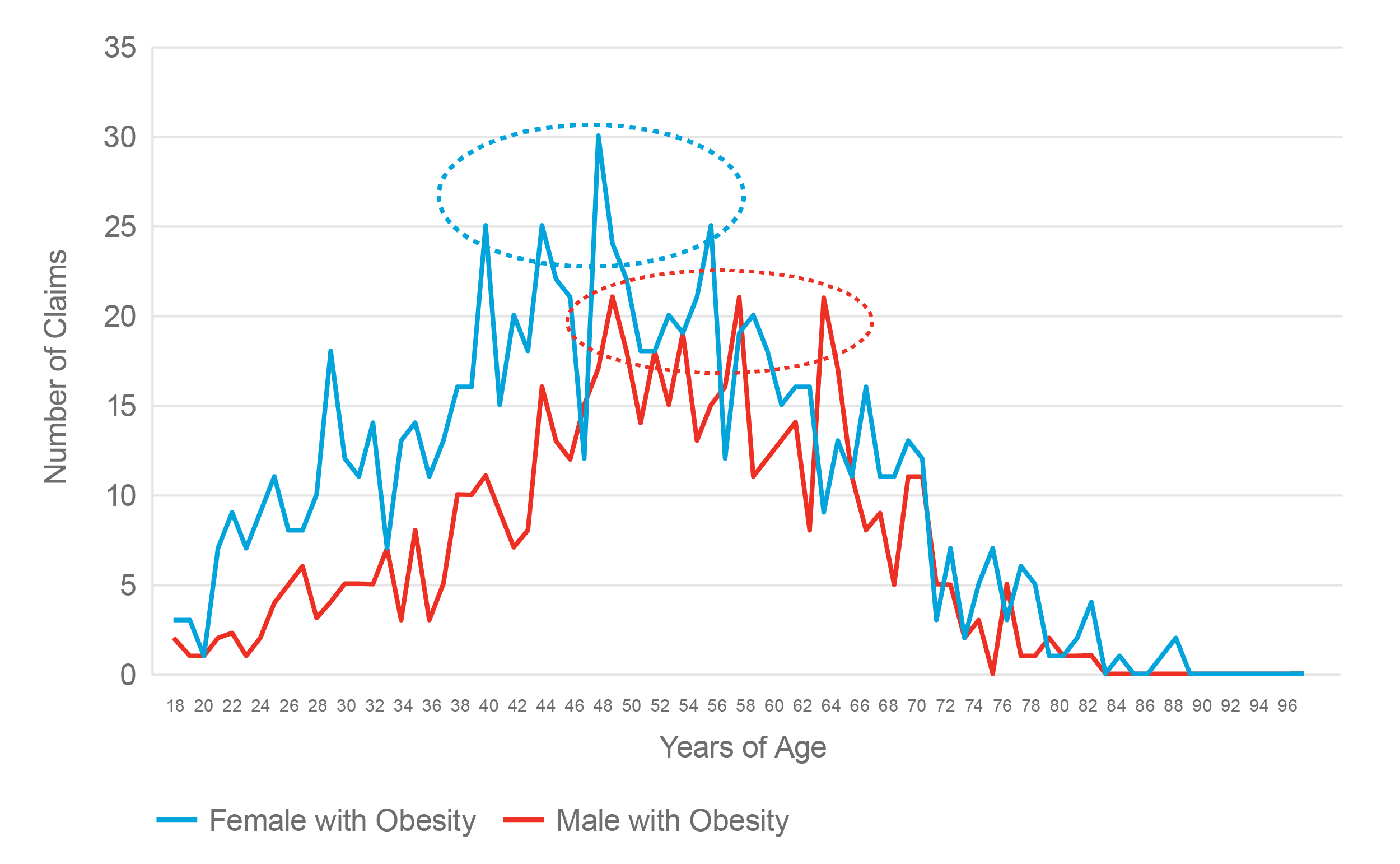
The number of female patients with an obesity comorbidity peaked between ages 40 and 56. The number of male patients with an obesity comorbidity peaked between ages 49 and 64—approximately eight or nine years later than the peak years for females.
Case Types, Factors that Contributed to Patient Harm, and Patient Injuries
We compared claims involving medical and surgical clinical services. The chart below outlines the case types, factors that contributed to patient harm, and patient injuries that had a 7 percent or greater differential between claims with obesity as a comorbidity and claims with no obesity comorbidity.
| Case Types | Obesity Comorbidity | No Obesity Comorbidity |
|---|---|---|
| Claims Against Medical Services | ||
| Diagnosis-related (failure, delay, wrong) | 40% | 32% |
| Claims Against Surgical Services | ||
| Improper management of surgical patient | 23% | 16% |
| Factors Contributing to Patient Injuries: | ||
| Claims Against Medical Services | ||
| Patient assessment issues | 45% | 34% |
| Failure or delay in obtaining a consult or referral | 19% | 12% |
| Claims Against Surgical Services | ||
| Patient assessment issues | 28% | 19% |
| Selection and management of therapy | 26% | 18% |
| Patient Injuries: | ||
| Claims Against Medical Services | ||
| Death | 51% | 37% |
| Embolism/thrombosis | 15% | 6% |
| Claims Against Surgical Services | ||
| Death | 18% | 7% |
Claims Analysis
A review of the statistical data in this analysis raised the following questions and concerns:
Did prejudice against individuals with obesity affect the quality of care for the patients in our study? Are other explanations for the differing results possible?
Examples of differences in contributing factors included:
- Inadequate patient assessments occurred at a higher rate (10 percent) in patients with obesity.
- Physician reviewers found problems with selection and management of therapy more frequently in patients with obesity (8 percent higher in surgical cases).
- Failure or delay in getting a consult occurred 7 percent more frequently when treating patients with obesity.
An increased frequency of serious injuries appeared to be a trend in this study:
- The frequency of patient deaths was 18 percent higher for patients with obesity.
- The frequency of cardiac or pulmonary arrest was 8 percent higher for patients with obesity.
- Embolism or thrombosis occurred 7 percent more often in patients with obesity.
Office Practice Considerations When Treating Patients with Obesity
We know that assessments and treatments of patients with obesity are affected by the characteristics of the office practice and the availability of tools and equipment designed for patients with obesity.
The Doctors Company’s patient safety risk managers survey hundreds of office practices each year. They identify the characteristics of practices that meet the needs of patients with obesity. This includes having appropriately sized furniture in the waiting areas and exam rooms and equipment—such as blood pressure cuffs, needles, and wheelchairs—designed for patients with obesity. Weight assessment tools are available, and these office practices provide weight education to patients. They also understand the importance of talking about weight with their patients, and they initiate the conversation early for better prevention and treatment.
Many factors inhibit practitioners from speaking frankly with patients about weight. As obesity rates increase, it is essential that practitioners recognize barriers to such communications. The American Medical Association has resources available to help practitioners discuss weight with patients.
Providing proactive care in an office setting to a patient who is overweight or has obesity may reverse a weight gain trend that could ultimately lead to serious health concerns. While bariatric surgery is a viable option, most patients prefer weight reduction over surgery. Treating patients with obesity with sensitivity involves attending to their needs for comfort, safety, and respect.
Obesity is one of many chronic health conditions afflicting patients that should be addressed. The person, not the obesity, should be the focus of treatment. As with any patient with a chronic health condition, a relationship with a respectful, caring practitioner forms the bedrock of good medical care.
Frequently Asked Questions
Patient Safety Strategies
- Have open and clear communications. Start the conversation in the exam room, and address weight management with your patients. Warn patients with obesity of all the hazards associated with being overweight, including the nature and frequency of possible medical or surgical complications.
- Document discussions you have with a patient regarding the need for weight loss.
- Provide intensive patient management. Follow patients with obesity to determine levels of adherence to medical recommendations and document in the medical record. Monitor evidence-based treatments and change approaches if the patient is not successful in achieving goals. Working with your patients can help them achieve weight control and reduce their chances of being harmed.
- Determine the appropriate setting for an invasive procedure. Consider the level of postoperative monitoring necessary to reduce the chance of an airway obstruction.
- Develop criteria for preoperative management of patients with obesity. Suggest a delay in elective surgeries, with weight loss as a goal when a patient does not meet recommended criteria. When in doubt, do not perform elective procedures.
- Obtain assistance from other specialties. Prior to surgery, refer patients to consultants (e.g., bariatric medicine, endocrinology, and anesthesia) to thoroughly assess the patient’s condition.
- Strengthen the informed consent process. Discuss and document the risks, benefits, and alternatives to treatment.
For assistance in addressing any patient safety or risk management concerns, contact the Department of Patient Safety and Risk Management at (800) 421-2368 or by email.
Resources
American College of Surgeons, Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program
American Medical Association, Person-First, Preventive Approach Needed to Tackle Obesity
American Society for Metabolic and Bariatric Surgery
Centers for Disease Control and Prevention, Overweight & Obesity
World Health Organization, Obesity and Overweight Fact Sheet
The guidelines suggested here are not rules, do not constitute legal advice, and do not ensure a successful outcome. The ultimate decision regarding the appropriateness of any treatment must be made by each healthcare provider considering the circumstances of the individual situation and in accordance with the laws of the jurisdiction in which the care is rendered.
J12427 06/20
